Understanding Phlebitis: Symptoms, Causes, and When to Seek Help
If you have ever noticed a warm, tender, or reddened area along a vein in your leg or arm, you may have experienced phlebitis. The term simply refers to inflammation of a vein, and while it is extremely common, many people are unsure of what causes it, how to recognize it, or when it crosses the line from a minor inconvenience into something that requires prompt medical attention. Understanding the basics of phlebitis can help you protect your vein health and know when it is time to call a doctor.
What Is Phlebitis?
Phlebitis occurs when a vein becomes inflamed, most often in the legs. Sometimes the inflammation develops on its own, and other times it is accompanied by a blood clot, a condition known as thrombophlebitis.
Superficial thrombophlebitis involves inflammation and/or clotting in veins just beneath the skin's surface. It is usually uncomfortable or even painful, but much less dangerous than a DVT. Deep vein thrombosis (DVT) involves a clot developing in the deeper veins of the leg. DVT can become life-threatening if a clot breaks free and travels to the lungs, causing a pulmonary embolism. Understanding which condition you may be dealing with is essential for getting the right care at the right time. It is recommended to consult your doctor in these cases, because the symptoms of superficial phlebitis can sometimes be difficult to distinguish from the symptoms of DVT.
Common Symptoms of Phlebitis versus DVT
Many people first notice phlebitis as a localized area of discomfort along a visible vein. Symptoms can vary, but some of the most frequently reported signs include:
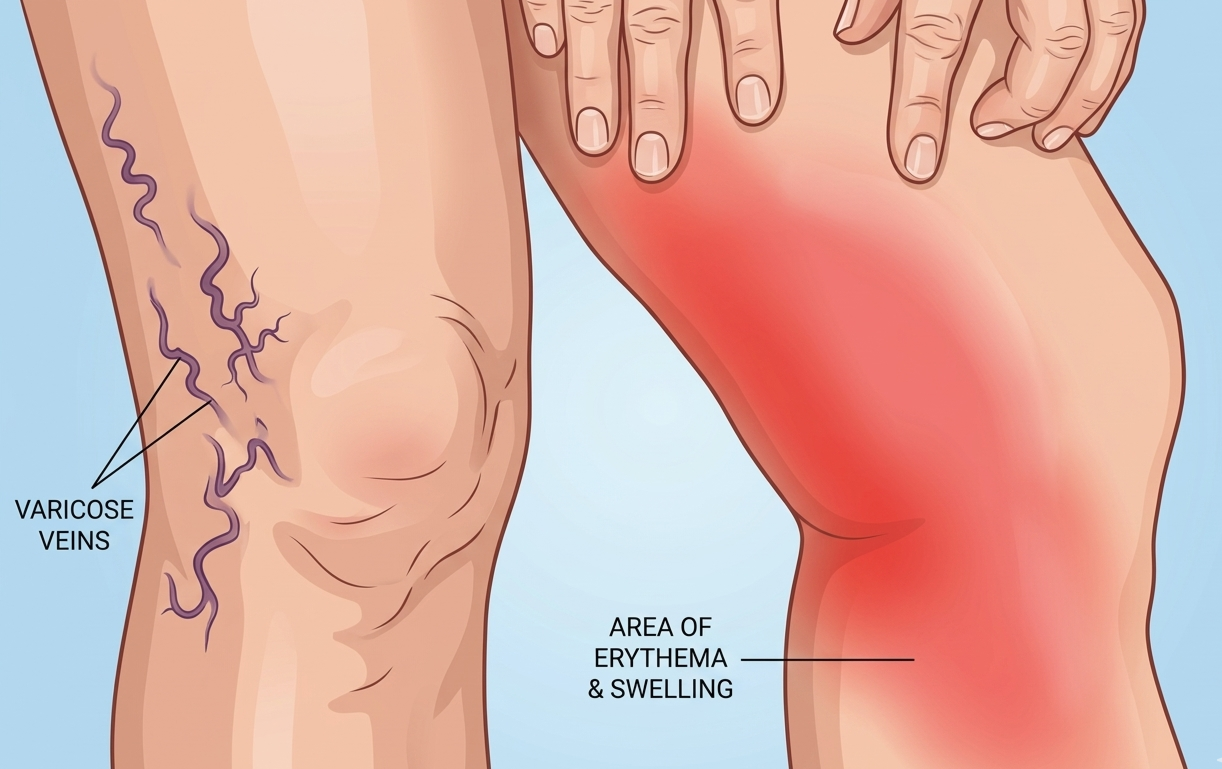
Redness, warmth, and tenderness along the path of a vein
A firm, cord-like feeling beneath the skin where the vein is inflamed
Swelling in the surrounding area, or in more serious cases, throughout the entire limb
Pain or a throbbing sensation that may worsen when standing or walking
Skin discoloration over the affected vein
When deep veins are involved, the symptoms may be more diffuse, including widespread leg swelling, heaviness, cramping, or, in urgent situations, sudden shortness of breath or chest pain. These symptoms should prompt you to seek medical attention right away.
What Causes Phlebitis and/or DVT?
Superficial phlebitis and DVT share some risk factors. They can be caused by one or more contributing factors that irritate the vein wall, slow blood flow, or increase the tendency for blood to clot. Some of the most common causes and risk factors include:
IV lines, injections, or direct trauma to a vein
Varicose veins, which are already dilated and prone to inflammation
Prolonged immobility from long flights, bed rest, or recovery after surgery
Smoking, dehydration, or obesity
Pregnancy and hormonal changes, including estrogen-containing birth control or hormone replacement therapy
Inherited clotting disorders such as Factor V Leiden
Cancer and certain cancer treatments
People with multiple risk factors should be especially mindful of changes in their legs and should not hesitate to seek evaluation if symptoms arise.
How Is Phlebitis or DVT Diagnosed?
When you visit a healthcare provider with suspected blood clots, the evaluation typically begins with a thorough history and physical examination. Your clinician will look for visible signs of inflammation and assess your risk factors. To confirm or rule out a blood clot, they may order aduplex ultrasound, which uses sound waves to visualize the veins and evaluate blood flow in real time. In some cases, a D-dimer blood test may also be used as part of the diagnostic process, particularly when DVT is suspected. For patients with recurrent or unexplained blood clots, additional lab work may be ordered to screen for underlying clotting disorders or other conditions.
Treatment Options
The approach to treatment depends on whether the condition is superficial or involves deeper veins. For uncomplicated superficial phlebitis, treatment usually focuses on reducing inflammation and supporting healthy circulation. Doctors often recommendcompression stockings to promote blood flow, along with leg elevation to reduce swelling. Over-the-counter anti-inflammatory medications like ibuprofen can help manage pain, and warm compresses applied to the affected area offer additional comfort. Applying an ice pack for 15 to 20 minutes several times a day can also be effective in managing the discomfort of superficial phlebitis. Staying gently active with light walking is encouraged to keep blood moving and help prevent clot formation.
In cases of DVT, the treatment plan becomes more involved. Anticoagulation therapy with blood thinners is often necessary to prevent clots from growing or traveling to the lungs. DVT always requires prompt medical treatment and careful follow-up to reduce the risk of pulmonary embolism.
When to Seek Medical Help
Knowing when to escalate your care can make a significant difference in outcomes. You should contact your healthcare provider or seek emergency services right away if you experience:
Sudden shortness of breath, chest pain, or coughing up blood (call 911)
Significant swelling of an entire limb
Fever, chills, or rapidly spreading redness over a vein
A history of DVT or pulmonary embolism with new or recurring symptoms
Phlebitis located near the groin or other deep vein junctions
Early evaluation and treatment are key to preventing serious complications and protecting your long-termvascular health.
Prevention Tips
While not all cases of blood clots can be prevented, there are practical steps you can take to lower your risk. Staying physically active,maintaining proper hydration, wearing compression stockings if recommended by your doctor, and avoiding prolonged periods of sitting or standing can all help support healthy blood flow. If you smoke, quitting is one of the most impactful changes you can make for your veins. For individuals with known risk factors, discussing preventive strategies with a vein specialist is a smart step toward staying ahead of potential problems.
The Bottom Line
While superficial phlebitis is usually a mild, self-limiting irritation, DVT is a medically urgent condition that demands immediate attention. If you notice a warm, red, tender vein or unexplained leg swelling, do not wait to get evaluated. Early diagnosis and targeted treatment can prevent complications and help you get back to feeling your best. To learn more about your vein health or to schedule a consultation,contact the specialists at Elmore Medical today.
Elmore Medical Vein & Laser Treatment Center is the premier vein specialty medical practice in the Central Valley. Dr. Mario H. Gonzalez and his staff offer years of experience and medical expertise that you won’t find anywhere else. Contact us to set up a consultation appointment.